Dense breast education
Understanding the screening and risk implications of dense breast tissue and advancing education on the topic to address knowledge gaps.

Mammography remains the standard of care in screening for breast cancer and has been proven to reduce the mortality rate (1).
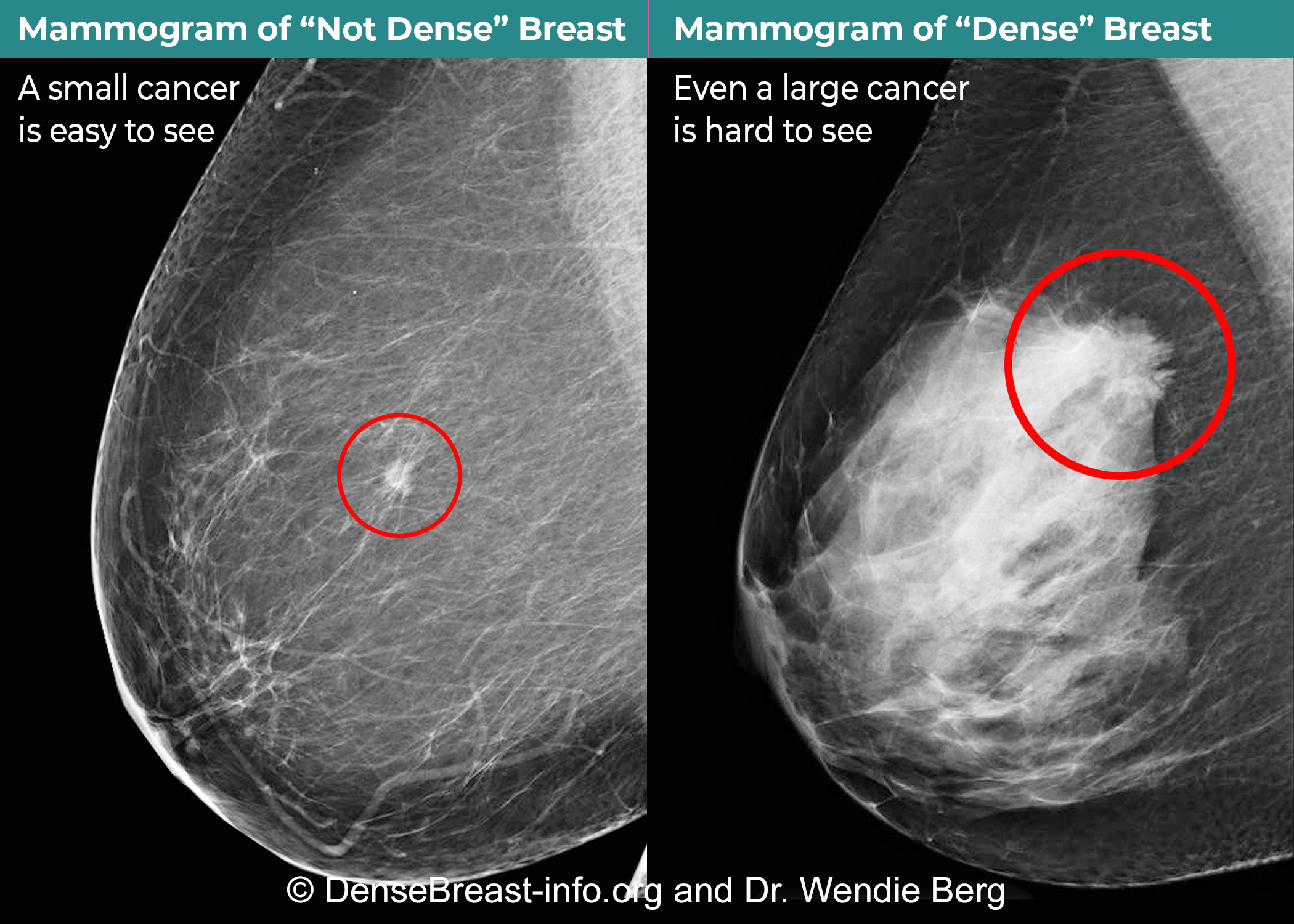
However, in dense breasts, cancers can be hidden/obscured on mammography (2)(3) (figure 1) and may go undetected until they are larger and more likely to present with clinical symptoms (4). Breast density has also been identified as the most prevalent risk factor for developing breast cancer (5).
Women with dense breasts are both more likely to develop breast cancer and more likely to have that cancer missed on a mammogram (6).
Figure 1. Cancer on a mammogram of a fatty versus a dense breast
What is dense breast tissue?
Breasts are made of fat and glandular tissue, held together by fibrous tissue. The more glandular and fibrous tissue present, the ‘denser’ the breast. Whilst dense breasts are normal and common, dense breast tissue makes it more difficult for radiologists and reporting radiographers to detect cancer on a mammogram.
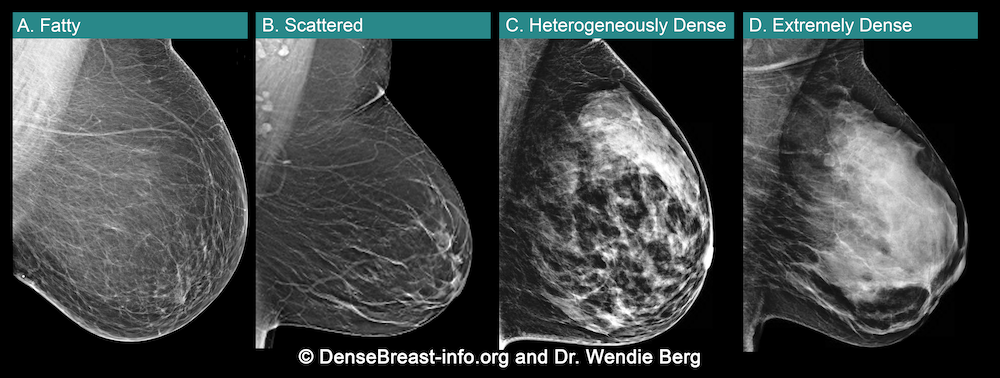
Breast density is determined through a mammogram and described as one of four categories (figure 2): A) Fatty, B) Scattered, C) Heterogeneously Dense, D) Extremely Dense. Breasts that are C) heterogeneously dense, or D) extremely dense are considered ‘dense breasts’ (figure 2).
Figure 2. The Breast Imaging Reporting and Data System (BI-RADS) categories of breast density
(American College of Radiology, ACR)
About Dense Breasts
Breast density has nothing to do with how breasts look or feel. On a mammogram, dense breast tissue displays as white or light grey, and the denser the tissue, the ‘whiter’ the mammogram. This matters because cancerous tumours also display as white on mammograms. Trying to find a cancer in a dense breast is like looking for a ball of cotton in a snowstorm. As density increases, the ability of a mammogram to show cancer decreases and the risk of developing breast cancer increases.





NHS Breast Screening Programme
Currently in the UK, women aged 50-70 are invited to routine screening mammograms every three years, and women over 70 years can self-refer. Though dense breasts affect the likelihood that a cancer will be masked and increases a woman’s risk for developing breast cancer, breast density is not part of UK data collection. A woman’s breast density is not assessed, not recorded in medical records, nor reported to her. For symptomatic women undergoing diagnostic tests, this may differ.
In many European countries, in population routine screening programmes, asymptomatic women’s breast density is assessed, recorded, and the woman’s personal breast density category is included in the mammography report. If the mammogram determines ‘dense’ breasts these women are offered supplemental ultrasound screening to help the radiographer or radiologist better interpret the breast images. A UK multicentre study, Breast Screening Risk Adaptive Imaging for Density (BRAID), is comparing breast scans to diagnose small breast cancers in dense breasts. The trial is focused on women within the standard breast screening programme who are found to have radiographically dense breast tissue. Women are invited to participate if ‘a high amount of dense tissue’ is determined on the mammogram.
Breast density educational resources
DenseBreast-info.org/Europe is the world’s leading website about dense breasts (figure 3). This medically sourced resource is the collaborative effort of world-renowned experts in breast imaging and medical reviewers. A growing number of medical organisations, including the European Federation of Radiographer Societies (EFRS) and the Society of Radiographers link to the DenseBreast-info.org website, signposting members to educational resources.
Figure 3. Welcome to DenseBreast-info/Europe

Educational tools for European providers
The website features educational tools for European providers (figure 4) including a Density Primer, a Risk Model Tutorial, European Screening Decision Support tool, research on health professional knowledge gaps, a comprehensive list of FAQs and articles, authored by international breast density experts, on the topic.
Figure 4. European Providers
Educational resources for patients (figure 5) include a Question and Answer section, a video series, Let’s Talk About Dense Breasts and patient resources, including a Patient Fact Sheet in multiple languages.
Figure 5. European Patients
Breast screening guidelines
Breast screening guidelines (figure 6) are available by European country. Details include the type of screening programme, start/stop and interval information, as well as guidelines when dense breasts are determined. A comparative analysis table summarises the guidelines in each country.
Figure 6. Country/Screening Guidelines

News in Europe: The EUSOBI recommendations
Population based breast screening guidelines vary across Europe. In the UK, asymptomatic women attending routine national breast screenings receive mammography alone. In some countries (e.g. Austria, Croatia, Hungary, France, Serbia, Spain, Switzerland) screening guidelines for women with dense breasts include that they be offered supplementary ultrasound following a mammogram.
Following recent magnetic resonance imaging screening trials there is cumulating evidence which confirms that women with dense breasts are underserved by screening with mammography alone (7) (8). In March 2022, new recommendations were issued in Breast cancer screening in women with extremely dense breasts by the European Society of Breast Imaging (EUSOBI) (9) highlighting the growing evidence, particularly the results of a randomised, multicentre controlled study, the Dense Tissue and Early Breast Neoplasm Screening (DENSE) Trial (7) (8).
The European Society of Breast Imaging 2022 recommendations now step away from the one-size-fits all approach of mammography that is currently adopted by most European screening organisations and advocates for tailored screening programmes. There is compelling evidence that the new recommendations enable an important reduction in breast cancer mortality for these women.
Summary of the EUSOBI recommendations
EUSOBI’s summary graphic of the recommendations (figure 7).
In addition to recommended additional screening in women with extremely dense breasts, note that EUSOBI recommends that “women should be appropriately informed about their individual breast density in order to help them make well-balanced choices.”
EUSOBI acknowledges that it may take time before the new recommendations are implemented in Europe and that the level of implementation is dependent on the resources that are available locally.
It is important to emphasise that the EUSOBI recommendations highlighted in this article are not yet guidelines in Europe. Of course, it is hoped that in Europe, national breast screening committees try to implement these recommendations as soon as possible to benefit women.
Figure 7. Screening in women with extremely dense breasts. Recommendations of the European Society of Breast Imaging









World Dense Breast Day
World Dense Breast Day (figure 8), sponsored by DenseBreast-info.org (DBI), is an annual social media education blitz which takes place the last Wednesday of every September. The purpose of the day is to raise awareness about dense breasts and share medically sourced educational resources for women and health providers.
In 2023, over 100 educational posts/videos were created by DBI and ran for 24 hours across social media channels. Analytics detailed participation from people in 64 countries, over 12.3 million people saw/read the posts and over 28,500 people clicked/liked or shared a post. The next #WorldDenseBreastDay will take place on 25 September 2024.
Figure 8. World Dense Breast DayTM

Take home message:
- Breast density can both hide cancers on a mammogram and increases the risk of developing breast cancer
- Women with dense breasts benefit from additional screening tests after their mammogram
- Breast density education and access to supplemental screening can mean the difference between an early or late-stage diagnosis
- Physicians should be educated and prepared to have patient conversations about breast density
For more information about breast density, visit: DenseBreast-info.org/Europe
References
1. Tabar L, Vitak B, Chen TH et al. Swedish two-county trial: impact of mammographic screening on breast cancer mortality during 3 decades. 2011. Radiology 2011;260:658-63
2. Hooley RJ, Greenberg KL, Stackhouse RM, Geisel JL, Butler RS, Philpotts LE. Screening US in patients with mammographically dense breasts: initial experience with Connecticut Public Act 09-41. 2012. Radiology 265:59–69
3. Kolb TM, Lichy J, Newhouse JH. Comparison of the performance of screening mammography, physical examination, and breast US and evaluation of factors that influence them: an analysis of 27,825 patient evaluations. 2002. Radiology 225:165–175
4. Roubidoux MA, Bailey JE, Wray LA, Helvie MA. Invasive cancers detected after breast cancer screening yielded a negative result: relationship of mammographic density to tumor prognostic factors. 2004. Radiology 230:42–48
5. McCormack VA, dos Santos Silva I. Breast density and parenchymal patterns as markers of breast cancer risk: a metaanalysis. 2006. Cancer Epidemiol Biomarkers Prev 15:1159–1169
6. Vourtsis A, Berg WA. Breast density implications and supplemental screening. 2019. Eur Radiol 29:1762-77.
7. Bakker MF, de Lange SV, Pijnappel RM et al. Supplemental MRI screening for women with extremely dense breast tissue. 2019. N Engl J Med 381:2091-102.
8. Veenhuizen SGA, de Lange SV, Bakker MF, Pijnappel RM, Mann RM, Monninkhof EM, Emaus MJ, de Koekkoek-Doll PK. 2021. https://doi.org/10.1148/radiol.2021203633 Radiology Vol. 299. No.2. Supplemental Breast MRI for Women with Extremely Dense Breasts: Results of the Second Screening Round of the DENSE Trial
9. Mann, RM, Athanasiou, A, Baltzer, PAT. et al. Breast cancer screening in women with extremely dense breasts recommendations of the European Society of Breast Imaging (EUSOBI). 2022. Eur Radiol 32, 4036–4045
Thank you to DenseBreast-info.org for permitting use of website images and selected content.

